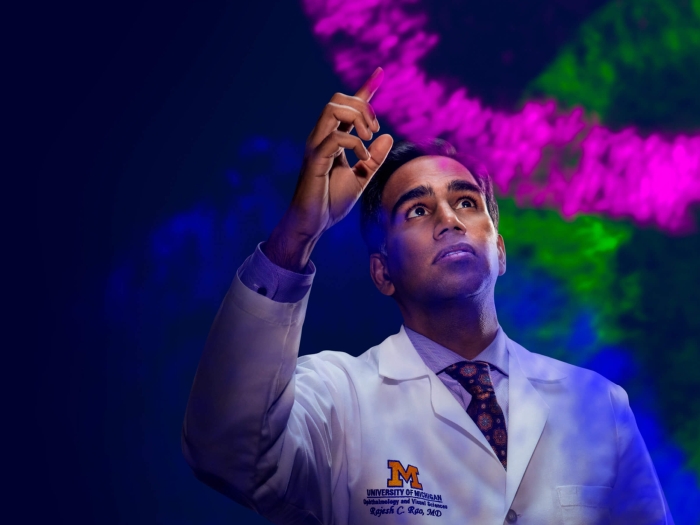
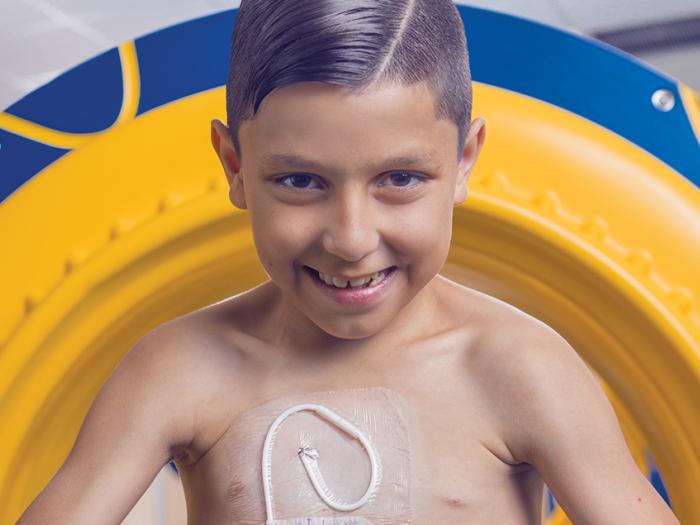
At Michigan Medicine, we believe there’s a difference between an answer and a Michigan Answer.
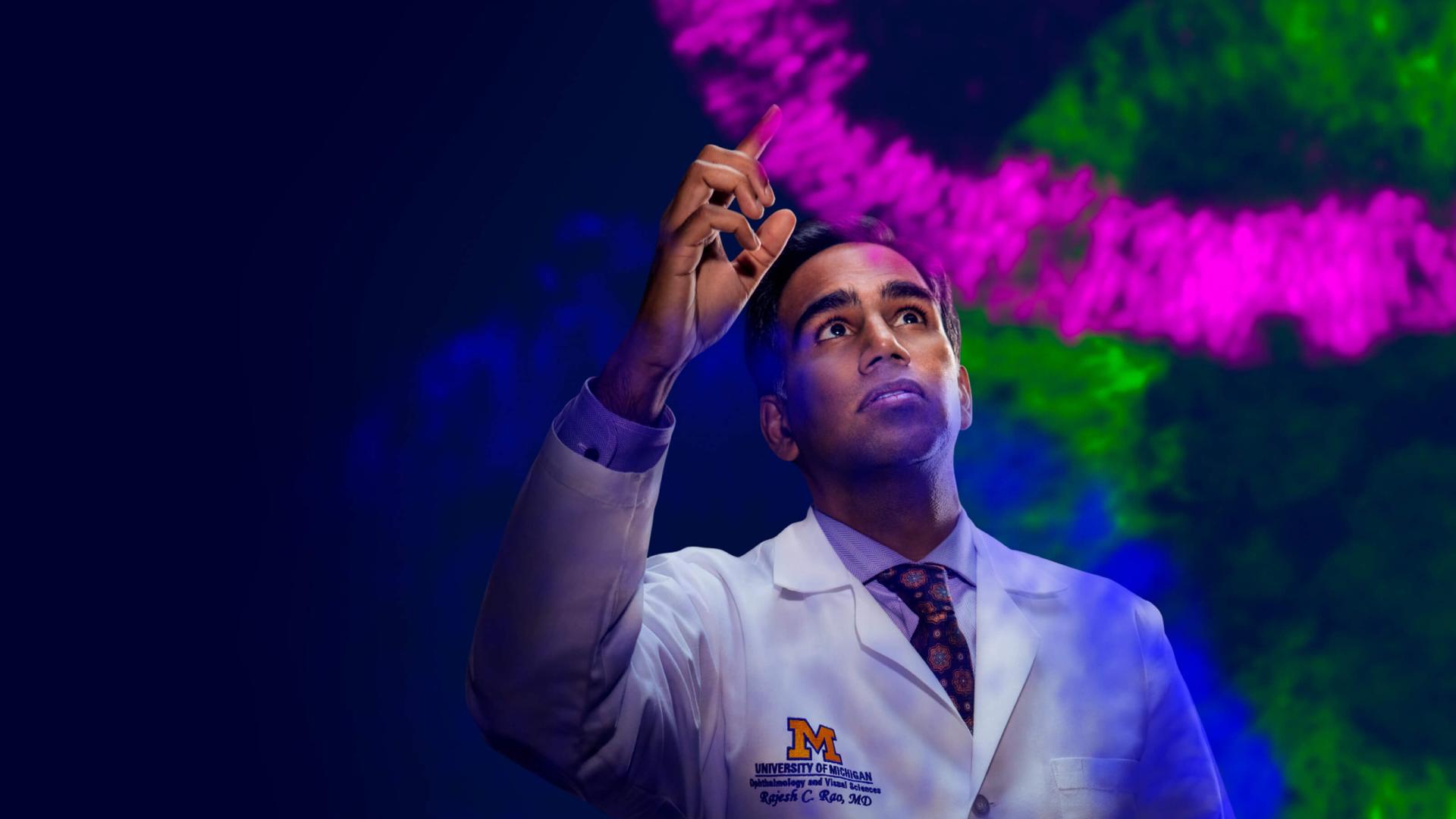

Michigan Answers are found where over 100 years of teaching, research and patient care intersect with an endless curiosity and passion for changing patients’ lives for the better. Michigan Answers come with confidence. Michigan Answers bring hope. Michigan Answers run toward the incurable and wrestle with the impossible until something new emerges. Michigan Answers are small steps and giant leaps, and the pathway to breakthroughs you’re waiting for.
Cancer care at Michigan's best hospital, Rogel Cancer Center.
Our Stories
The easiest way to understand what makes a Michigan Answer is to hear the stories of our patients, physicians, researchers, scientists, students and families. We hope these inspire you and give you hope for finding your own Michigan Answer.
Kristi Brown’s first pregnancy had been going even better than she hoped. Her medical appointments had all delivered good news. She and her husband, William, were happily preparing the baby’s room, all the while sharing their excitement with friends and loved ones.